Does a PAP Machine Help After a Heart Attack? (CPAP, APAP, BiPAP Explained)
If you’ve had a heart attack, you’ve probably been told to take your meds, watch your diet, and stay active. But there’s another big piece of recovery that many people miss:
How you breathe while you sleep.
For many heart attack survivors, sleep problems aren’t just annoying. They can be a real health risk—especially if you have sleep apnea.
In this article, you’ll learn:
What PAP therapy is (CPAP/APAP/BiPAP)
Why sleep apnea can stress the heart
How PAP may help after a heart attack
What the research really says
How to know if you should be tested
(Educational only. Always work with your cardiologist and sleep specialist for personal medical advice.)
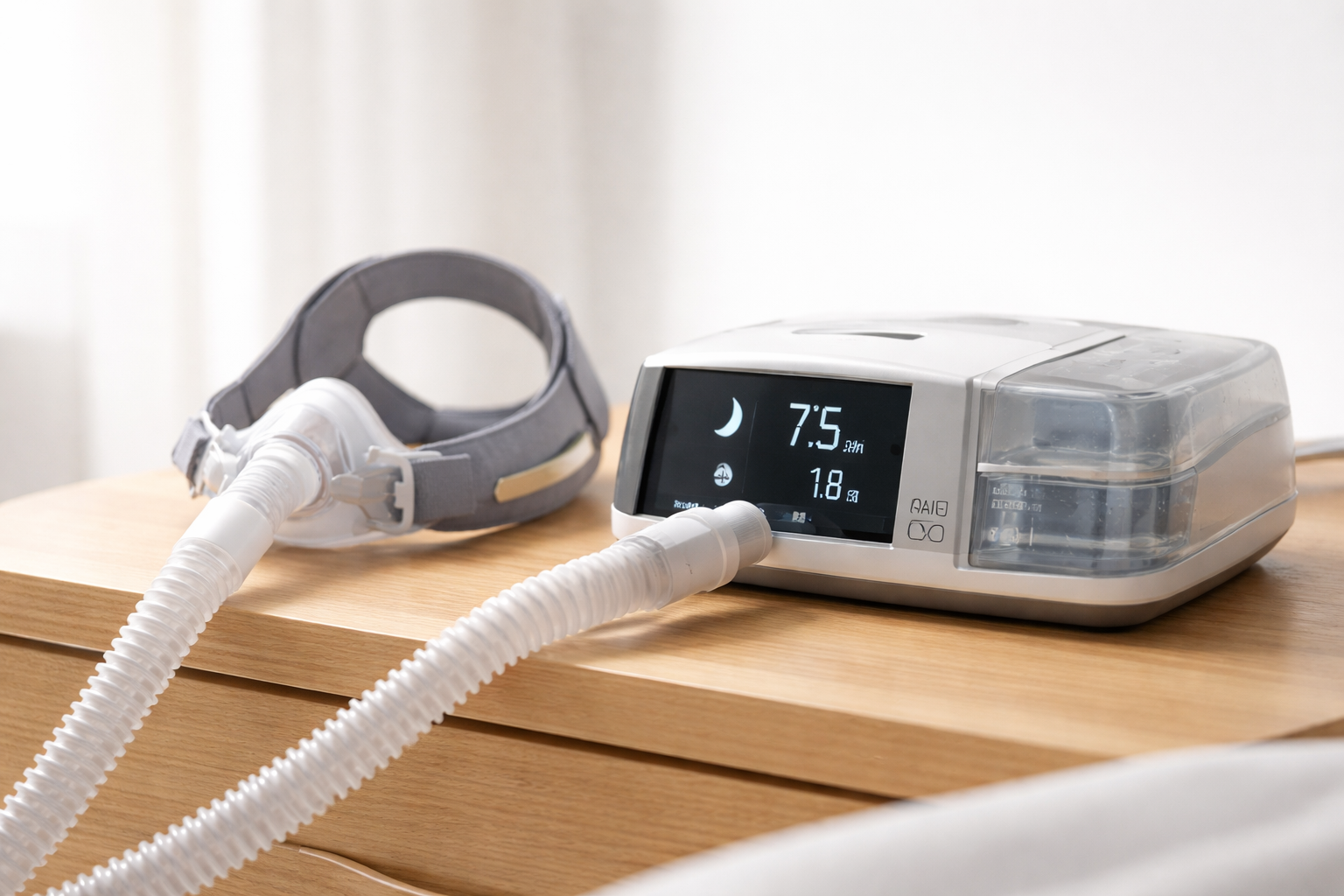
What is PAP therapy?
PAP stands for Positive Airway Pressure.
It’s a machine that gently pushes air through a mask while you sleep. This air pressure helps keep your airway open so you can breathe normally all night.
Common types:
CPAP (Continuous PAP): One steady pressure all night.
APAP (Auto CPAP): Adjusts pressure as your breathing changes.
BiPAP/BPAP: Higher pressure when you inhale and lower pressure when you exhale. This is used for certain breathing or comfort needs.
PAP is most often used to treat Obstructive Sleep Apnea (OSA).
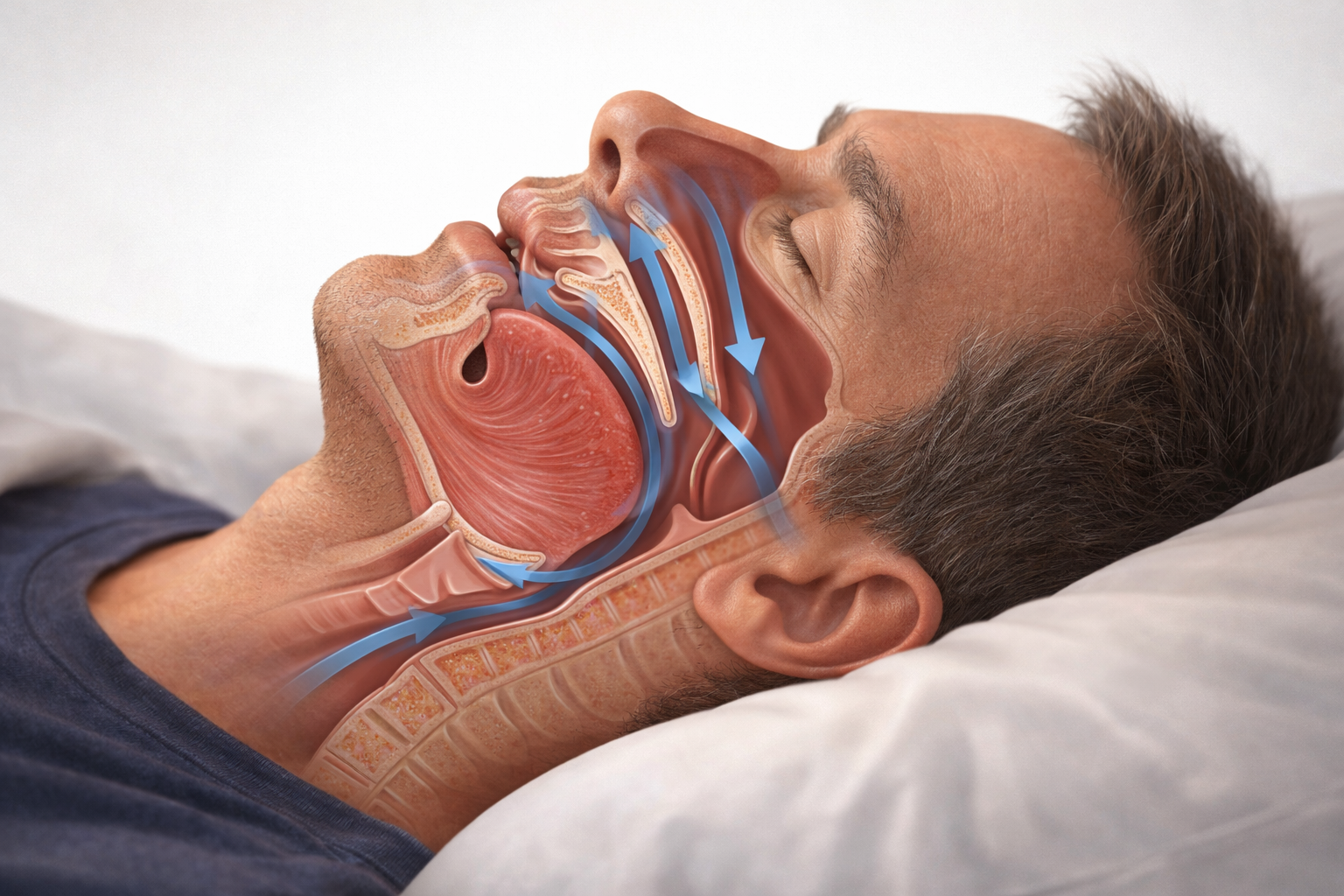
What is obstructive sleep apnea (OSA)?
OSA happens when the throat relaxes too much during sleep. The airway narrows or closes. Breathing slows or stops for short periods—over and over.
Your brain notices the danger and briefly wakes you up to restart breathing. Many people don’t remember waking up, but the body still gets stressed.
Signs of sleep apnea include:
Loud snoring
Choking or gasping during sleep
Waking up tired (even after 7–9 hours)
Morning headaches
Dry mouth
Sleepiness during the day
High blood pressure that’s hard to control
OSA is strongly linked with high blood pressure and heart disease.
Why sleep apnea can be dangerous after a heart attack
After a heart attack, your heart is healing. It needs stable oxygen and calm, steady recovery.
Sleep apnea can work against that healing in a few big ways:
1) Oxygen drops can strain the heart
With OSA, oxygen levels can drop many times per night. That means the heart has to work harder to deliver oxygen to the body.
2) Stress hormones surge during the night
Each breathing pause can trigger a “fight-or-flight” response. This raises:
Heart rate
Blood pressure
Stress hormones (like adrenaline)
Over time, this can keep the cardiovascular system on high alert.
3) Blood pressure can rise (especially at night)
Nighttime blood pressure should normally dip. Sleep apnea can prevent that dip, which is a problem for heart recovery.
Research and expert statements note CPAP adherence is linked with better blood pressure control, including nighttime blood pressure.
4) Rhythm problems can become more likely
Sleep apnea is associated with heart rhythm issues like atrial fibrillation. PAP may help reduce this stress in some people.
So… does PAP help someone who has had a heart attack?
If you have sleep apnea: PAP can be a big win
When a heart attack survivor has OSA, PAP often helps by:
Keeping oxygen levels steadier
Reducing nighttime “stress surges”
Improving sleep quality
Reducing daytime fatigue
Helping blood pressure control in many patients
Many patients also report:
Less snoring
Fewer nighttime bathroom trips
Better energy
Better mood and focus
But what about preventing another heart attack?
This is where people get confused—because the science is mixed.
A major trial (SAVE) found that adding CPAP to usual care did not reduce major cardiovascular events overall in a broad group of patients with heart/cerebrovascular disease and OSA.
Another large study in acute coronary syndrome patients (ISAACC) also found no significant reduction in cardiovascular events overall with CPAP in the group studied.
But here’s the key detail:
In several analyses, people who used CPAP more consistently (often defined as ≥4 hours/night) appeared to do better.
And newer research suggests that some “high-risk” sleep apnea patterns may benefit more than others (not everyone has the same kind of OSA).
Plain English summary:
PAP is not a magic shield that guarantees you’ll never have another heart event. But if you truly have sleep apnea and you use PAP consistently, it can reduce strain on your heart and may improve risk in certain people—plus it often improves quality of life.
Who should seriously consider a sleep apnea test after a heart attack?
You should talk to your doctor about testing if you have any of these:
Sleep signs
Loud snoring
Pauses in breathing (someone notices)
Gasping/choking at night
Severe daytime tiredness
Heart signs
High blood pressure that’s hard to control
Atrial fibrillation or other rhythm problems
Heart failure symptoms
A heart attack at a “young” age or without clear explanation
The American Heart Association has emphasized that sleep apnea is common in people with cardiovascular disease and often goes unrecognized.
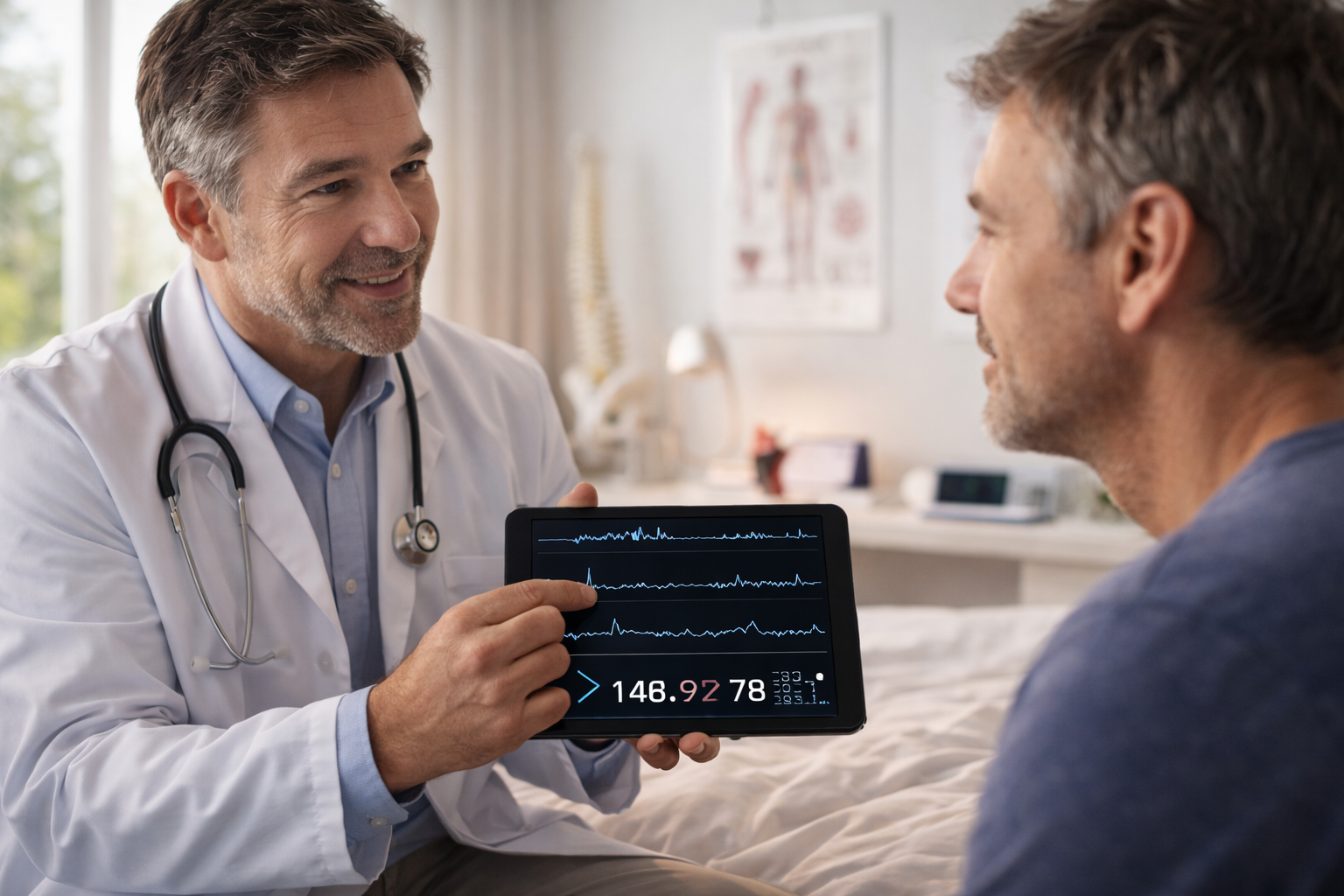
What happens during diagnosis?
Most people are diagnosed using:
Home sleep test (common, easier)
Sleep lab study (more detailed)
You’ll get numbers like:
AHI (Apnea-Hypopnea Index): how many breathing events per hour
Typical ranges:
Mild: 5–14
Moderate: 15–29
Severe: 30+
Your clinician will also look at oxygen drops and how your heart responds during sleep.
How to get the best results from PAP (this part matters)
PAP only helps if you actually use it.
Here are practical tips we teach patients in respiratory care:
1) Aim for “every night, all night”
In research, better outcomes often show up when people average around 4+ hours/night or more.
2) Fix mask problems quickly
Most people quit PAP because of mask leaks, dryness, or discomfort—things that are usually fixable by changing mask style or fit.
3) Manage dryness and congestion
Humidification, heated tubing, saline rinse, and the right mask can make a huge difference.
4) Track your progress
Many machines show nightly usage and mask leak. That feedback helps you improve.
Important safety note: not every “PAP-like” therapy fits every heart patient
Most heart attack survivors with obstructive sleep apnea can use CPAP/APAP safely under medical guidance.
But if someone has central sleep apnea and heart failure with reduced ejection fraction, certain advanced devices (like adaptive servo-ventilation, ASV) have shown harm in one major trial and require careful specialist guidance.
This is one reason a proper sleep evaluation matters.
The Cardio Natural perspective
Make it stand out
Whatever it is, the way you tell your story online can make all the difference.
At Cardio Natural, we love strategies that:
Reduce the workload on the heart
Improve recovery habits
Support long-term energy and consistency
PAP therapy is not “just a sleep tool.” For the right person, it can be a heart recovery tool, because it stabilizes breathing, oxygen, and nighttime stress.
Simple action plan (start here)
Ask this question: “Could I have sleep apnea?”
Talk to your cardiologist or primary care doctor about a sleep study.
If diagnosed, commit to 30 days of consistent use and solve comfort issues early.
Keep doing the foundations: meds, walking, food changes, stress reduction, and follow-up care.
Call to action
If you’re recovering from a heart attack—or trying to prevent one—don’t ignore your sleep.
Follow Cardio Natural for practical, step-by-step heart health guidance that supports real life. And if you found this helpful, share it with someone who snores, wakes up tired, or is working on their blood pressure.
Your next step:
✅ Talk to your doctor about a sleep apnea test if any signs fit you.
✅ Then keep building your heart-healthy routine—one habit at a time.